Hydrotherapy offers a gentle yet highly effective way to manage chronic pain, particularly for conditions that may not respond well to traditional land-based exercise or medical treatments. Exercising in warm water reduces the effects of gravity, allowing your body to move with significantly less strain and discomfort.
The supportive environment of a therapeutic pool allows patients to perform movements that may feel difficult or painful on land. This helps improve mobility, strength, and confidence while reducing pain levels, making hydrotherapy an important part of many rehabilitation programs.
The Science Behind Water Therapy
Four Healing Properties of Water
Hydrotherapy works because of the unique physical properties of water:
Buoyancy
Water supports your body weight, reducing joint and tissue stress. Waist-deep water can reduce body weight by around 50%, while chest-deep water can reduce it by up to 70%. This allows people to move more freely and comfortably than they may be able to on land.
Hydrostatic Pressure
The natural pressure of water helps improve blood circulation and reduce swelling. It also supports lymphatic drainage, which assists in managing inflammation and fluid retention.
Water Resistance
Water provides gentle, consistent resistance in every direction. This allows you to build strength safely without placing excessive strain on joints or relying on heavy weights.
Warmth
Therapeutic pools are typically heated to relax muscles, reduce stiffness, improve tissue flexibility, and help reduce pain signals sent to the brain.
Pain Relief Mechanisms
Hydrotherapy supports pain relief through several biological and psychological pathways. Warm water helps relax muscles and reduce muscle spasms, which can interrupt ongoing pain cycles. Gentle exercise stimulates the release of endorphins — the body’s natural pain-relieving chemicals — which also help improve mood.
Research shows hydrotherapy can be particularly beneficial for individuals with fibromyalgia, helping reduce pain, stiffness, fatigue, anxiety, and depression symptoms.
Building Confidence Through Movement
Many people living with chronic pain develop a fear of movement, often due to concerns that exercise will worsen their symptoms. This fear can lead to reduced activity levels, muscle weakness, and increased pain over time.
Hydrotherapy provides a safe, supportive environment that helps rebuild confidence in movement. As patients gradually experience improved comfort and mobility, they often regain trust in their body’s ability to move without triggering significant pain.
Conditions That May Benefit from Hydrotherapy
Hydrotherapy can support a wide range of chronic pain conditions, including:
• Arthritis and joint degeneration
• Fibromyalgia
• Post-surgical rehabilitation
• Chronic back and neck pain
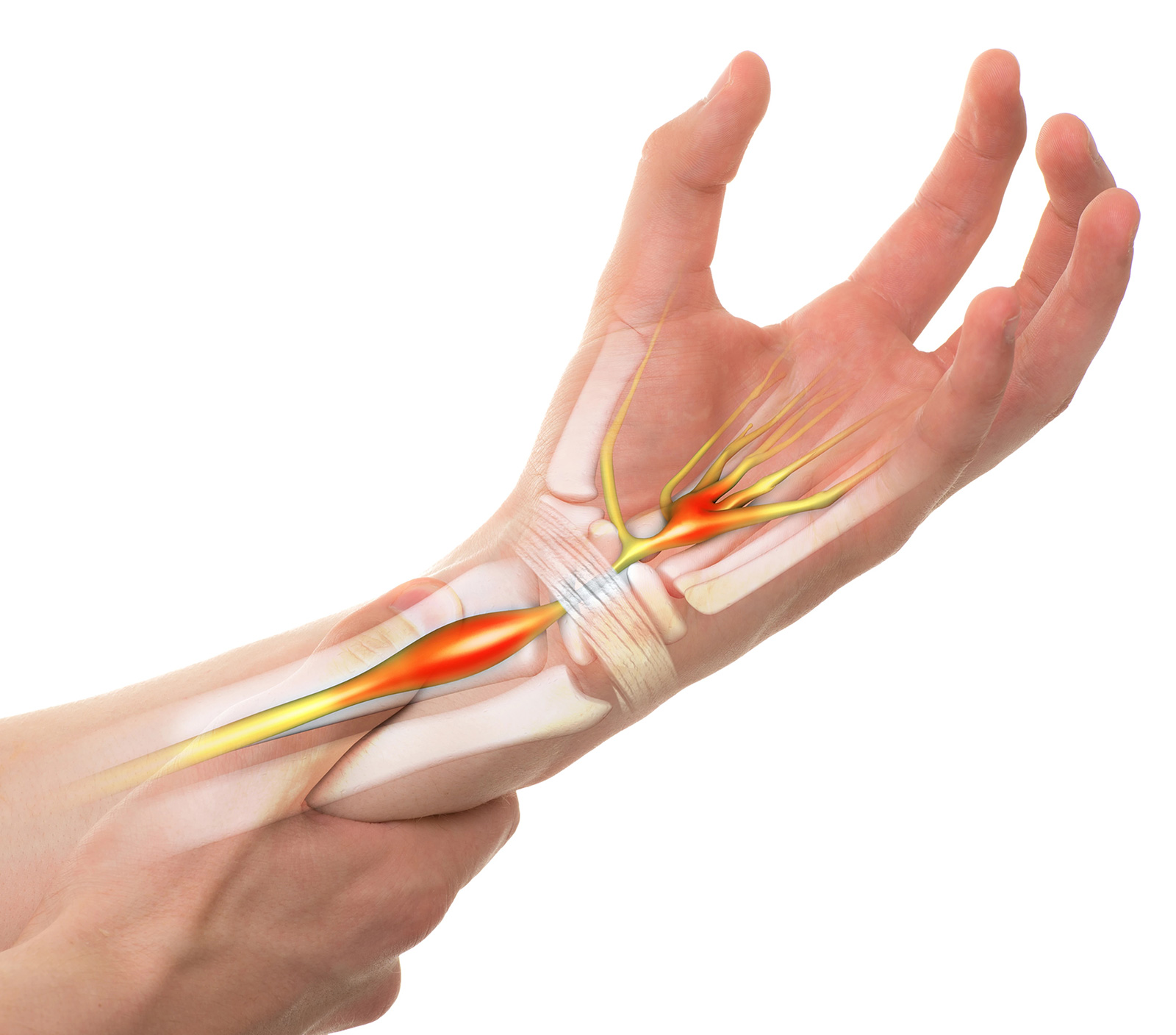
• Neuropathy and nerve-related pain
• General musculoskeletal pain conditions
By improving both physical function and mental wellbeing, hydrotherapy can play an important role in long-term pain management.
What to Expect During Hydrotherapy Sessions
Hydrotherapy programs are tailored to each individual’s condition, goals, and physical capacity. Sessions typically run for around 30 minutes and are often scheduled weekly over a 5–6 week period, depending on your treatment needs.
Exercises are guided by a physiotherapist in a heated pool maintained at approximately 33–36°C. The water depth is carefully selected to provide stability, support balance, and allow controlled movement.
Sessions usually begin with gentle walking and stretching exercises before gradually progressing to strengthening, balance, and mobility training as confidence and pain tolerance improve.
Maximising Long-Term Results
Hydrotherapy is most effective when combined with a broader rehabilitation plan. This may include:
• Pain education
• Psychological support strategies
• Individualised home exercise programs
• Strength and conditioning exercises
A multidisciplinary approach helps patients build long-term self-management skills, reduce flare-ups, and maintain independence in daily activities.